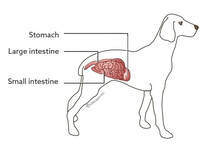
in Dogs
By Renee Schmid, DVM & Ahna Brutlag, DVM, MS, DABT, DABVT Pet Poison HelplineWhile a favorite and healthy snack for people, grapes, raisins and currants can cause kidney failure in dogs. Raisins can commonly be found in combination with other foods, potentially increasing the risk of exposure as compared with grapes and currants. The toxicity concern is the same.
What types of grapes and raisins are toxic to dogs?
Poisoning has occurred in dogs following ingestion of seedless or seeded grape varieties, commercial or homegrown grapes, red or green grapes/raisins, organic or non-organic, and grape pressings from wineries. Foods containing grapes, raisins, and currants (such as raisin bran cereal, trail mix, granola mix, baked goods) are all potential sources of poison. Grape jellies, grape juice and wine do not appear to cause a toxicity concern.
What is the toxic dose?
Unfortunately, there is no well-established toxic dose for any of these fruits but there are two principles to keep in mind: 1) Dogs are more likely to become poisoned if they ingest large amounts of fruit and, 2) there appears to be ‘individual’ sensitivity in dogs. Some dogs appear to be tolerate to small doses of fruit without consequence while other dogs may develop poisoning after eating just a few grapes or raisins. At this time, there is no way to predict which dogs may be more sensitive.
Why are raisins, grapes, and currants toxic?
Currently, it is not known why these fruits are toxic. Over the years, there has been speculation as to whether the toxicity may be due to a mycotoxin (a toxic substance produced by a fungus or mold) or a salicylate (aspirin-like) drug that may be naturally found in the grape, resulting in decreased blood flow to the kidneys. More recently, it has been considered that tartaric acid may be the cause. However, to date, no specific toxic agent has been clearly identified. Since it is currently unknown why these fruits are toxic, any exposure should be a cause for potential concern.
What should I do if my dog eats grapes or raisins?
If you suspect that your pet has eaten any of these fruits, contact your veterinarian, Pet Poison Helpline or an animal poison control service immediately. Since there are still many unknowns associated with this poisoning, it is better not to take any risks when it comes to your dog's health. As with any toxin, the sooner the poisoning is diagnosed and treated, the less dangerous it will be for your pet, and the less expensive therapy will be for you.
What are the symptoms of grape or raisin toxicity?
The most common early symptom of grape or raisin toxicity is vomiting. which is generally seen within 24 hours hours following ingestion. Lack of appetite, lethargy, and possibly diarrhea can be also seen within the next 12-24 hours. More severe signs are not seen for 24-48 hours after ingestion – often after acute kidney damage has already begun. Signs of acute kidney failure include nausea, lack of appetite, vomiting, uremic (ammonia odor) breath, diarrhea, abdominal pain, excessive thirst, and excessive urination. As poisoning progresses, the kidneys will stop functioning and the dog may not be able to produce urine. Following this, the dog's blood pressure often increases dramatically. The dog may lapse into a coma due to a buildup of substances which the kidneys usually eliminate from the body through urine. Once the kidneys have shut down and urine output has dropped,the prognosis is poor.
How is grape/raisin poisoning diagnosed?
Unfortunately, the symptoms of grape or raisin poisoning are non-specific and early signs are similar to a variety of things including simple dietary indiscretion (eating foods that should not be eaten). More severe signs are similar to kidney failure from other causes. Your veterinarian will base a diagnosis of this poisoning on a history of eating grapes, raisins, currants, or the presence of pieces of grapes or raisins in the dog's vomit. Your veterinarian may also recommend diagnostic tests such as a complete blood count (CBC), a serum biochemistry profile, and a urinalysis to assess the amount of damage to the kidneys. The test results will help determine the dog's likelihood of recovery.
How is this poisoning treated?
The goal of treatment is to block absorption of the toxins and prevent or minimize damage to the kidneys. The best treatment is to decontaminate the dog right away by inducing vomiting and administering activated charcoal. This helps to prevent absorption of the toxin from the stomach or intestines. As grapes and raisins stay in the stomach for a prolonged period of time, inducing vomiting is very important (even up to 4-6 hours after ingestion). Following decontamination, more treatment might be necessary including aggressive intravenous fluids to help support/protect the kidneys in hopes of minimizing damage to them. Drugs used to control nausea or vomiting, to help maintain blood flow to the kidneys, and to control blood pressure may also be administered.
"The goal of treatment is to block absorption of the toxins and prevent or minimize damage to the kidneys."
Ideally, dogs should be hospitalized on intravenous fluids for 48 hours following ingestion. Affected animals may need to be hospitalized for several days. During treatment, your veterinarian will monitor the dog's kidney function levels daily to assess the response to treatment and determine whether the treatment needs to become
more aggressive. Blood work may also be repeated 1-2 days after going home. This is to make sure kidney function levels have not increased.
What is the prognosis following poisoning from grapes or raisins?
Prognosis depends on many factors, including how significant the ingestion is, how soon the patient was decontaminated, whether or not the patient has already developed kidney failure, how soon treatment was initiated, and whether the clinical signs and kidney function levels have improved since treatment began. If a dog only ate a few grapes or raisins (depending on the size of the dog) and received immediate treatment, the prognosis is excellent. If the kidneys are damaged and no urine is produced, the prognosis is poor, and death is likely. The kidneys have very little ability to regenerate or repair themselves. Once they are damaged, they will not function as well as they did before the episode. When in doubt, seek treatment right away by contacting your veterinarian or Pet Poison Helpline for advice. Your veterinarian will estimate the prognosis for your dog based on symptoms, individual situation, and response to treatment.
How can I prevent this problem?
Keep all grapes, raisins, currants, or foods containing these fruits, out of reach of your pets. Do not share any food that may contain grapes or raisins with your dog, and especially do not use grapes as treats for your dog. While one grape may not cause a problem for most dogs, it is a good idea to avoid this habit and risk a potential poisoning.
What other common foods are toxic to dogs?
Onions, garlic, alcohol, chocolate, cocoa, macadamia nuts, fattening foods, and foods containing the sugar alcohol sweetener xylitol, can also be fatal.
Are other animals at risk?
Grape and raisin poisoning has only been identified as a problem in dogs. Since there are still many unknowns associated with this poisoning, it would be a good idea to avoid giving any grapes and raisins to your dog or any other pet.
Pet Poison Helpline, an animal poison control center based out of Minneapolis, MN is available 24/7 for pet owners and veterinary professionals that require assistance treating a potentially poisoned pet. The staff provides treatment advice for poisoning cases of all species, including dogs, cats, birds, small mammals, large animals and exotic species. As the most cost-effective option for animal poison control care, Pet Poison Helpline’s fee of $65 per incident includes follow-up consultations for the duration of the poison case. Pet Poison Helpline is available in North America by calling 800-213-6680. Additional information can be found online at www.petpoisonhelpline.com